This is Part 2 of the series on fibre. In case you missed it, have a look at the previous part: 👉 Part 1: How To Feed Your Gut?
Eating a high-fibre diet is now mainstream advice.
Walk down any grocery aisle and you'll see products proudly proclaiming their high fibre content. Doctors and nutritionists alike recommend a diet high in fibre to maintain digestive health and prevent constipation. The WHO recommends at least 25 grams of fibre a day.
This advice is so widely accepted that it seems almost heretical to question it.
The conventional wisdom that fibre is good for your bowel movements is so ingrained in our subconscious that it can even be uncomfortable to think that the opposite might be true. We've been and continue to be bombarded by advertisements, product labels, nutritionists and other people telling us that we need to eat fibre.
But there is little hard science to back it up.
Let's look at a bit of history first.
❗️ Subscribe for free to receive new posts and support my work.
High fibre intake hasn't always been mainstream dietary advice.
In the late '60s, Denis Burkitt, an Irish surgeon, returned to the UK from Africa, where he had been studying cancer. He observed that traditional African societies had a much lower prevalence of "Western diseases" and attributed this difference to their diet and lifestyle.
He was greatly influenced by another surgeon, Thomas Cleave.
Cleave researched the negative health effects of consuming refined carbohydrates, like sugar and white flour. While it's clear to us now that sugar is harmful, this was a new idea at the time. Burkitt merged Cleave's research with his own observations. He began examining the Western diet compared to traditional African diets, leading to the development of the fiber hypothesis.
Burkitt, who became known as "FibreMan", managed to get his hypothesis into the mainstream.
The hypothesis was that a diet rich in plant matter kept our ancestors free of disease, a notion based on Cleave's observations. He noted that the modern diet contained a significant increase in refined carbohydrates, which were low in fibre. Cleave suggested that the overconsumption of these carbohydrates led to modern diseases such as bowel cancer and heart disease.
But Burkitt didn't endorse Cleave's theory.
He changed it to his own, claiming that it was the lack of fibre in the carbohydrates that caused the diseases.
It's a subtle but crucial distinction.
Burkitt's fibre theory fell on fertile ground in the USA in the 60's and 70's.
Around the same time, Ancel Keys led a campaign against saturated fat, arguing that it was a major cause of cardiovascular and heart disease. Despite a lack of hard evidence and relying mainly on observational studies, he persuaded the US government to recommend that the American public reduce their intake of saturated fat and increase their intake of carbohydrate-rich foods.
Burkitt's fibre theory fitted well with Ancel Keys' fat theory.
Furthermore, the sugar industry paid scientists to produce reports that pointed the finger at fat, not sugar, as the cause of heart disease.
By the 1970s, the stage was set for both Burkitt's and Keys' theories to lead the US government, through Senator McGovern's committee, to issue the first official dietary guidelines. These guidelines, not surprisingly, favoured carbohydrates over fats.
Companies like Kellogg's were promoting wholegrain cereals as healthy long before McGovern's dietary guidelines or Burkitt's fibre hypothesis.
However, their motivation was rooted in religious belief rather than scientific evidence. John Kellogg, founder of the Kellogg's brand, was a Seventh-day Adventist, a religion that advocates a vegetarian diet. He believed that eating bland foods, such as whole wheat, could prevent disease and discourage masturbation, which his faith considered evil.
Cereal companies seized the business opportunity in the changing dietary landscape by marketing breakfast as the most important meal of the day. This strategy, along with prevailing theories about fibre and fat and societal changes such as women entering the workforce, cemented high-fibre cereals as a breakfast staple.
That's history, but let's get back to what we know about fibre today.
Support for high-fibre diets is often based on epidemiological studies that show correlation rather than causation. While these studies are useful for generating hypotheses, they often fall short of providing solid evidence.
We cannot simply jump from “fibre is associated with fewer health problems' to 'fibre prevents health problems”.
But does fibre help prevent constipation?
It's well known that fibre adds bulk to the stool because it's undigested material that needs to be expelled. Constipation not only means having to defecate infrequently, but having to defecate with difficulty and pain.
So the question is: does increasing stool bulk with more fibre actually help this condition?
Think of being stuck in a traffic jam. By adding fibre, you are adding more cars to an already congested traffic jam. You may have more cars on the road, but the congestion will still be there and may get worse.
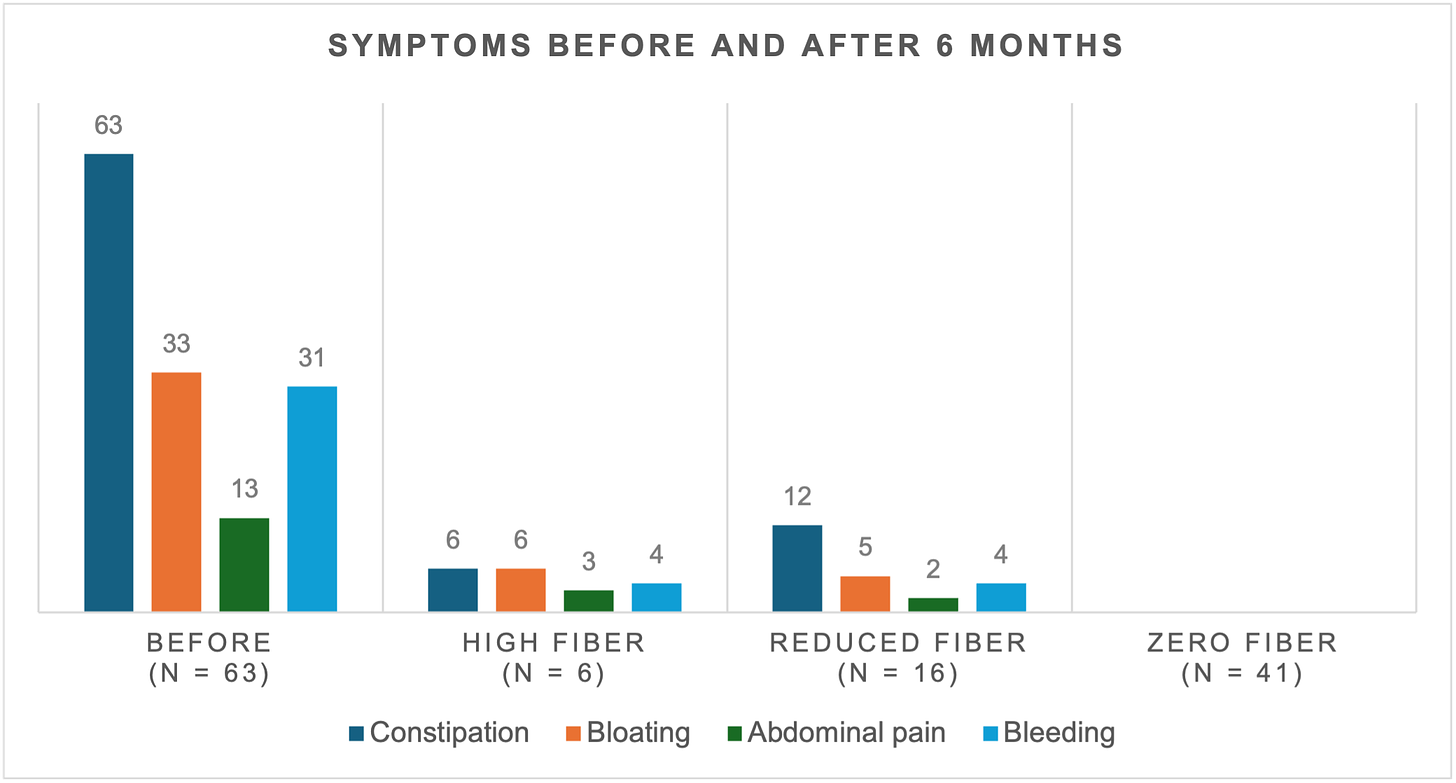
This prospective, interventional study looked at zero-fibre, reduced-fibre and high-fibre diets. It enrolled healthy people who were already eating a high-fibre diet, but were still struggling with constipation and other digestive symptoms.
After 6 months, the results were surprising - at least in terms of conventional wisdom.
Only the zero fibre diet completely eliminated constipation, bloating and pain.
At the start of the study, patients were asked to stop eating fibre for 2 weeks, but to keep their eating habits as close to normal as possible (for example, swapping brown rice for white) to maintain their typical carbohydrate and protein levels.
After 2 weeks, they were told to continue with as little fibre as they felt comfortable with in the long term. The patients were followed up after the first month and again after six months. As you can see from the graph, out of 63 patients, 41 stayed on the fibre-free diet, even though it's the most restrictive.
Clearly, the complete elimination of chronic digestive problems can make it easier to stick to a diet.
Those who went back to eating fibre experienced digestive problems, which were most common in the high-fibre group.
The researchers also learned that some patients did not adhere to a fibre-free diet for reasons such as vegetarianism, psychological discomfort from avoiding fibre, and constant media and peer pressure to consume fibre.
This highlights how our dietary choices are strongly influenced by our social context.
We tend to follow mainstream advice because we think it must be true.
After all, this is the 21st century, so we must have figured out something as elementary as fibre and defecation, right?
If you enjoyed reading this, please like ❤️ and leave a comment 💬 below.
Your engagement helps more people discover this post on Substack 🙏.